Purpose
The Corinthian Plan is a self-funded, church-plan health program of Mennonite Church USA designed to ensure that pastors and church staff have access to quality healthcare regardless of the financial capacity of their congregation. Rooted in the Anabaptist value of mutual aid, we share both the costs and the commitment to one another’s well-being.
The Corinthian Plan is built on the principle that no congregation should carry the cost of caring for its pastor alone. When you participate, you’re not just buying a health plan — you’re joining a community of Mennonite churches that share costs, share risk, and share responsibility.

Why Choose The Corinthian Plan?
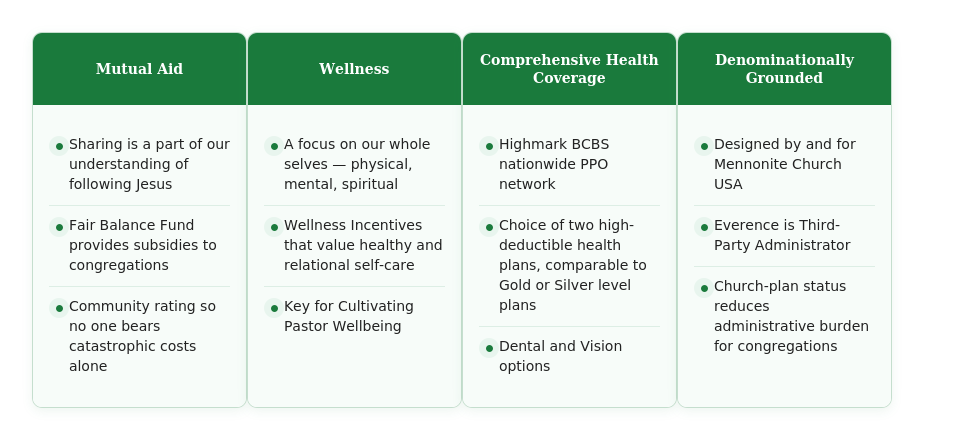
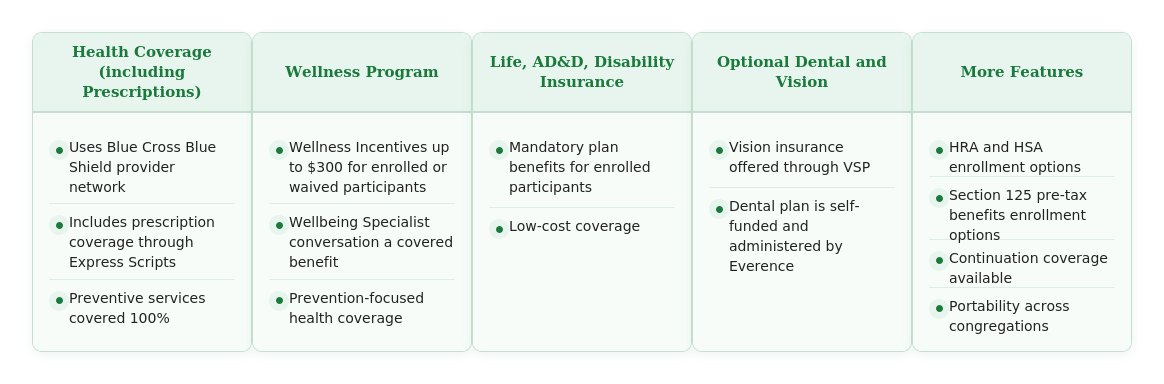
Benefits Offered
Where Would You Like to Start?
News & Updates
Watch Recent Webinar
Click button below to watch a recording of the January 2026 webinar on Engaging Our Grief and Finding Resilience.
Earn up to $300! New Wellness Incentive Year
Earn up to $300!
Wellness Incentives for the new cycle: March 1, 2026 – February 28, 2027





